CUHK
News Centre
CUHK’s study sees a rising trend of multiple myeloma incidence, particularly in older males from high-income countries
Multiple myeloma, lymphoma and leukaemia are the three major types of haematological malignancies. In Hong Kong, multiple myeloma is the third most common among them. According to Hong Kong’s Hospital Authority, there were 320 new cases of multiple myeloma in 2019, an increase of about 40% compared with a decade ago. The Chinese University of Hong Kong (CUHK)’s Faculty of Medicine (CU Medicine) has conducted a study with the Association of Pacific Rim Universities (APRU) to investigate the global distribution, risk factors and epidemiological trends of multiple myeloma. The results showed that the incidence of multiple myeloma was higher in high-income jurisdictions, and was closely related to the gross domestic product (GDP) per capita levels, the human development index (HDI) as well as the prevalence of physical inactivity, overweight and obesity rates, and diabetes.
The global incidence of multiple myeloma has also shown an obvious rising trend in recent years, particularly in older males from high-income countries. The researchers recommend that risk factor control and early cancer detection should be implemented for high-risk populations. Details of the study have been published recently in the top international medical journal The Lancet Haematology.
Multiple myeloma is more common in older male populations, with a higher incidence in high-income countries. Hong Kong’s incidence was more than twice of that in mainland China
Multiple myeloma is more common in the elderly and the male population. According to the Hospital Authority, over 60% of new multiple myeloma cases in 2019 were 65 years old or older, and 55% of them were males. Multiple myeloma is a clonal plasma cell neoplasm characterised by uncontrolled proliferation of mutated plasma cells within the bone marrow, leading to specific end-organ damage, especially in the cortical bone. It is called multiple myeloma because the cancer often affects several areas of the bone and marrow. Common symptoms include a persistent bone pain in the back or ribs, caused by bone resorbing damage; shortness of breath and tiredness caused by anaemia and kidney failure; and fevers due to immune deficiency.
To understand the most updated geographical distribution and identify high-risk population groups, the research team retrieved data from international databases such as the Global Cancer Observatory, WHO mortality database and WHO Global Health Observatory data repository, for the age-adjusted incidence, mortality and prevalence of different risk factors.
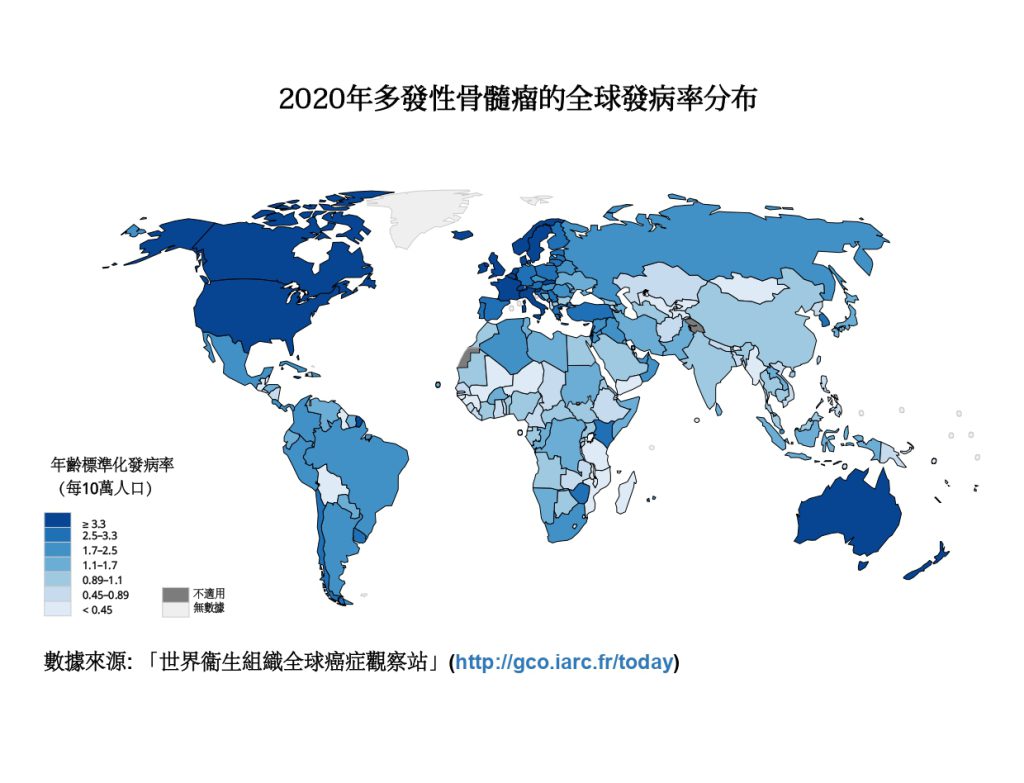
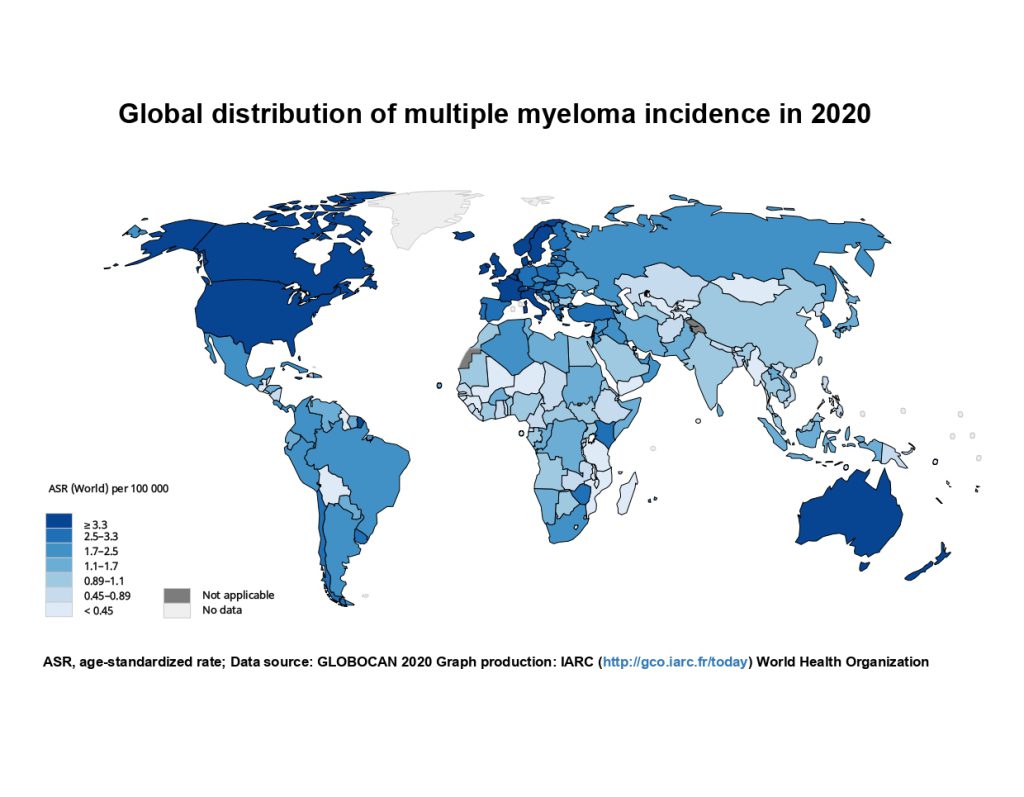
The researchers found that the disease burden of multiple myeloma varied across regions, with Australia and New Zealand having the highest incidence (4.9 per 100,000 population), followed by North America (4.8) and Northern Europe (3.8). The incidence in Hong Kong (2.0) was more than twice of that in mainland China (0.91), although the incidence was relatively low in East Asia (1.1). In addition, the disease burden of multiple myeloma was proportional to GDP, HDI and the prevalence of physical activity, excess weight, obesity and diabetes. This implies that a country or region with a higher level of those risk factors will have higher morbidity and mortality from multiple myeloma.
Global multiple myeloma incidence is on the rise, while the death rate is on the decline
Multiple myeloma has been rising globally over the past decade, particularly in developed economies. Using the “Average Annual Percentage Change (AAPC1)” for comparison, the largest increase in incidence rate among males was found in Turkey (5.6), followed by Germany (4.6) and Denmark (3.8). Among females, the largest increase was found in Denmark (3.8), followed by the United Kingdom (1.9). A relatively larger increase was found in males aged 50 years and older, which was most pronounced in Germany (6.7), followed by Denmark (3.9) and South Korea (3.3).
In contrast, the trend in mortality from multiple myeloma has been decreasing, especially in the female population.
Dr Huang Jun-jie, first author of the study and Post-Doctoral Fellow from The Jockey Club School of Public Health and Primary Care at CU Medicine, said, “The incidence and mortality of multiple myeloma vary by region, which may be related to detection and diagnosis ability, environmental and lifestyle factors, and the prevalence of metabolic diseases in each place. Our study provides the most up-to-date evidence on the global distribution, risk factors and trends of multiple myeloma. Future studies should explore the reasons behind these epidemiological transitions, so that they can provide insights on the cause and prognosis.”
Professor Martin Wong Chi-sang, the senior corresponding author of the study, from The Jockey Club School of Public Health and Primary Care at CU Medicine, added, “The overall incidence of multiple myeloma has been on the rise in recent years, but it is encouraging that the mortality rate has declined because of advances in and increased accessibility of treatment. This study also shows that the prevalence of physical inactivity, excess weight, obesity and diabetes are important drivers of the increase. Policy makers in different regions should implement evidence-based, targeted prevention strategies to control relevant risk factors.”
This study is a collaboration with Professor Mellissa Withers, the Director of the APRU Global Health Programme, Keck School of Medicine, University of Southern California. The APRU was established in Los Angeles in 1997 by the presidents of UCLA, Berkeley, Caltech and the University of Southern California. It now has a membership of 60 leading research universities from around the Pacific Rim. CUHK is an important member of APRU and Professor Martin Wong is currently the Co-Chairman of the Non-Communicable Diseases (NCD) Global Health Research Group for the network.
Study details can be found at: https://doi.org/10.1016/S2352-3026(22)00165-X
1 AAPC is a measure of the overall changes in cancer incidence or mortality for a specific period. For example, if the incidence AAPC of a certain cancer in a country is five for the past 10 years, it means that the incidence in that country increased 5% on average each year over the 10-year period.

CU Medicine has conducted a study with the Association of Pacific Rim Universities (APRU) to investigate the global distribution, risk factors and epidemiological trends of multiple myeloma. The results showed that the incidence of multiple myeloma was higher in high-income jurisdictions, and was closely related to the gross domestic product (GDP) per capita levels, the human development index (HDI) as well as the prevalence of physical inactivity, overweight and obesity rates, and diabetes. It is noted that multiple myeloma is more common in older male populations, and Hong Kong’s Incidence was more than twice of that in mainland China.
From right: Professor Martin WONG and Dr. HUANG Jun Jie from The Jockey Club School of Public Health and Primary Care at CU Medicine.